Nail Fungus Treatment, Causes and Prevention
What is nail fungus?
Nail fungus is a common condition in which fungi enters the nail area and infects the skin in between the nail and the skin. Toenail fungus and fingernail fungus are both prone to fungal infections. Once the infection grows in the nail bed, part the nail can become yellow or white. As bits of nail flake off and build up under the nail, the nail itself may split, crumble or separate from the skin. Nails will appear thicker than usual and may be uncomfortable when wearing certain shoes, in addition to being unsightly. While nail fungus medication exists, including home remedies for nail fungus, the condition can persist and be difficult to treat. Nail fungus, technically called onychomycosis, occurs more frequently in those over 60 or with diabetes but can affect anyone.
What are the signs of nail fungus?
With both toenail fungus and fingernail fungus, the infection begins as a pale yellow or white spot under the tip of your fingernail or toenail. You may notice additional symptoms as the condition progresses such as:
- Thicker than usual nails
- Spreading discoloration at the top of nails
- Ragged nail edges from crumbling
- Distorted nail shape
- Slight odor from the affected nail(s)
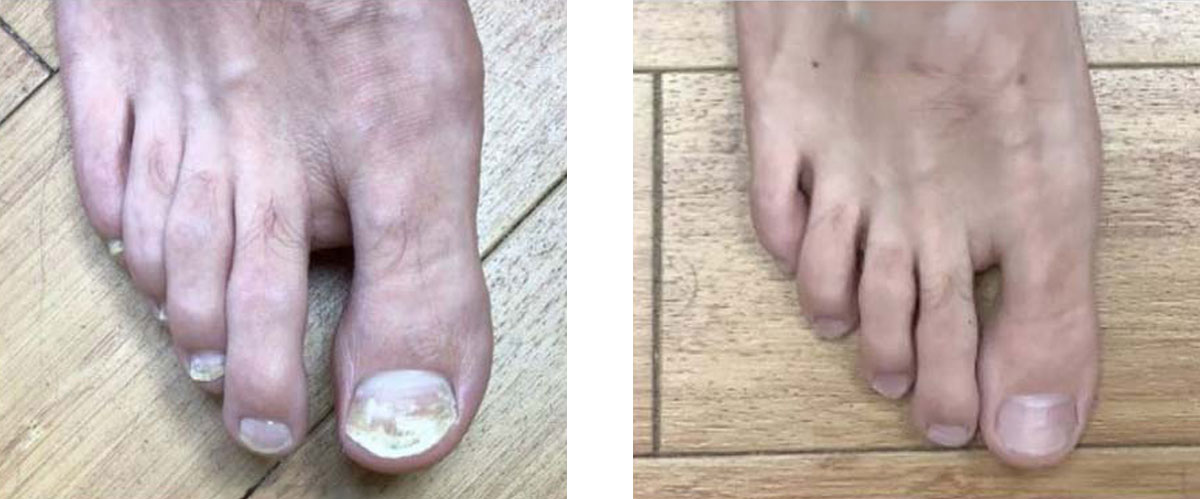
Toenail fungus before and after treatment
What are the different types of nail fungus?
Distal subungual onychomycosis (DSO)
This onychomycosis represents the most common type of fungal nail infection. The same organisms that create athlete’s foot also create DSO. It begins with infected skin under the nail bed. As debris builds up under the nail, the nail may crumble or even separate from the skin. Despite the prevalence of distal subungual onchomycosis, it remains difficult to treat.
Read more about Distal Subungual Onychomycosis
White superficial onchomycosis (WSO)
White superficial onchomycosis affects the uppermost layer of the toenail or fingernail. White spots appear on the top layer of the nail, which may cause the surface of the nail to appear chalky. WSO is easily treated, as the infection does not reach between the nail and the skin.
Candida onychomycosis (CO)
Though uncommon, candida onychomycosis affects the nail and the skin adjacent to the nail, which makes it painful. It might cause the skin or nail to turn white, green or brown and it’s possible for the nail to separate from the nail bed. This type of infection can be painful due to tender or swollen skin near the affected area.
What causes nail fungus?
Fungi developing in between the nail and the skin typically causes nail fungus. Yeast or mold can occasionally trigger an infection. Several factors can increase your likelihood of developing toenail fungus or finger nail fungus:
- Being older, which correlates into slower growing nails
- A history of athlete’s foot
- Sweating often and/or heavily
- An underlying skin condition such as psoriasis
- Walking around barefoot in locker rooms, gym showers and by swimming pools
- Patronizing nail salons that do not sterilize equipment
- Circulation problems, diabetes or a weakened immune system.
How do I treat nail fungus?
Nail fungus treatment can be tricky but various remedies exist. Nail fungus medication that can be obtained without a prescription includes antifungal creams and gels found at most local pharmacies. Nail fungus treatment should begin at the first sign of infection. The use of tea tree oil, apple cider vinegar, antibacterial mouthwash and snakeroot have also been touted by some a natural nail fungus medicine when applied daily for several weeks. Your doctor can also prescribe an anti-fungal topical drug that goes on like nail polish or antifungal pills to treat your onychomycosis. In severe cases your doctor may opt to remove all or part of the toe nail and a new nail will grow in its place.
How can I prevent nail fungus?
There are several nail health tips to reduce the likelihood of developing nail fungus:
- Wear shoes made of breathable material and not all leather
- Change your socks during the day
- Wear sweat wicking or sweat absorbing socks
- Opt for 100% cotton socks
- Treat shoes with antifungal powers
- Wear waterproof shoes around swimming pools and common shower areas
- Trim nails straight across and file edges and thick areas
- Disinfect nail clippers after each use
- Patronize nail salons that sterilize their equipment
Do I need to contact a doctor about nail fungus?
If you suffer from nail fungus, don’t let it fester. There are cases where nail fungus can grow severe enough to warrant a doctor visit. If nail fungus becomes painful, it may indicate a severe infection that can permanently damage your nails. It may also lead to other serious infections that spread to other parts of you body should you have a suppressed immune system. If your nails appear to be infected and you are experiencing pain, see a doctor. Often, over the counter remedies will just not be strong enough and you’ll need a dermatologist's care to prescribe an anti-fungal topical ointment which will help speed healing. Dermatology Physicians of Connecticut doctors are experts at handling severe cases of nail fungus.
Note: If you have diabetes, other exacerbating factors exist. You may have reduced nerve supply and/or blood circulation in your feet and toes. Diabetics also have a greater risk of Cellulitis, a bacterial skin infection. Because nail fungus can lead to other complications, diabetics who suspect a fungal infection should see a doctor at the earliest sign.