Melasma
What is Melasma?
Many women – and some men – notice gradual appearance of patchy tan to brownish pigmentation on the face. When the melanocytes (cells within the skin) produce too much pigmentation, melasma occurs.
What causes melasma?
The exact cause of melasma is unknown, however, this condition appears to be influenced by both hormones and sun. We know the sun is necessary for development of melasma and patients often note the patches become darker or more prominent with sun exposure.
Hormonal changes also can trigger melasma. In fact, melasma is often called “the mask of pregnancy.” In addition to pregnancy related hormone changes, oral contraceptives are often implicated as well. Sometimes melasma can appear without any known hormonal influence, suggesting also a possible hereditary tendency.
Can I treat my melasma?
Melasma is not dangerous, but patients are often self-conscious about their appearance and wish to treat it.
Sun protection is the most important component of any treatment plan for melasma. Any progress made with treatment can be reversed by later sun exposure. Avoid sun exposure, if at all possible, and wear a wide brimmed hat if the sun can’t be avoided. Apply broad spectrum sunscreen (SPF of 30 or higher) every day and plan to reapply at regular intervals. Be aware there is UV exposure even through car windows! Vigilant sun protection can actually result in improvement as well as prevention of melasma.
Melasma may fade naturally with time; however, treatment is available for persistent pigmentation. Non-prescription preparations containing botanical and natural lightening agents may fade mild cases. Your dermatologist can prescribe creams containing hydroquinone, tretinoin or azelaic acid. Chemical peels, light and laser therapies are effective for restoring even skin tone and correcting skin discoloration. Your dermatologist can tailor a treatment regimen to best meet your needs.
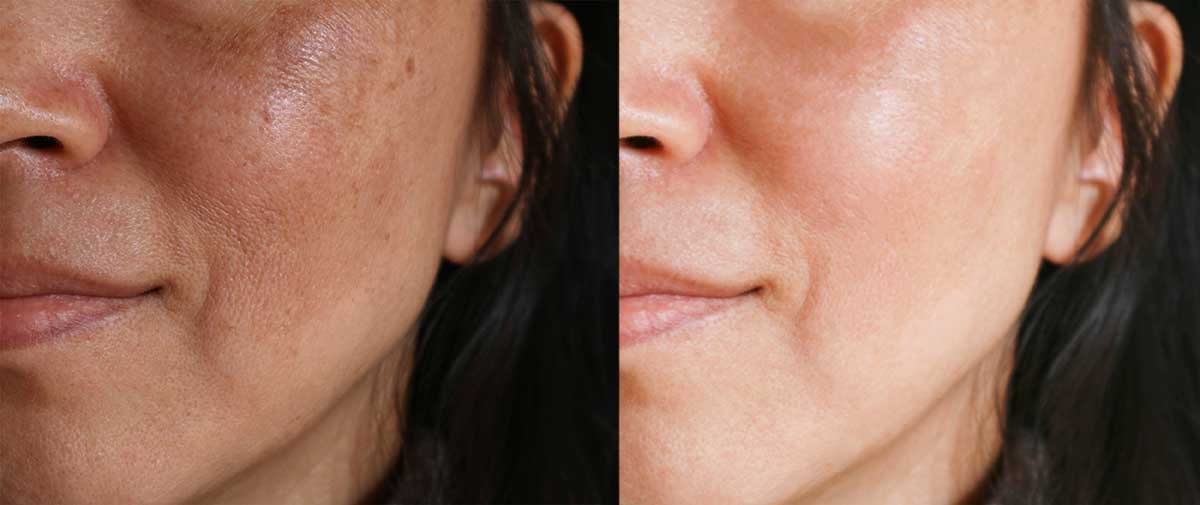
Before and after treatment