Skin Cancer Screening and Treatment in Connecticut
What causes basal cell carcinoma?
Basal cell carcinoma (BCC) is primarily caused by prolonged exposure to ultraviolet (UV) radiation from the sun or artificial sources like tanning beds. UV radiation damages the DNA in skin cells, particularly in areas frequently exposed to sunlight such as the face, neck, and arms. Over time, this damage accumulates, leading to mutations that trigger the uncontrolled growth of basal cells in the skin, resulting in the formation of tumors characteristic of BCC. Other factors such as a history of sunburns, a weakened immune system, and genetic predisposition can also contribute to the development of basal cell carcinoma. Protecting the skin from excessive sun exposure through measures like sunscreen use, protective clothing, and seeking shade can significantly reduce the risk of developing this common type of skin cancer. Regular skin checks and early detection are crucial for effective treatment and prevention of complications associated with basal cell carcinoma.
What does basal cell carcinoma look like?
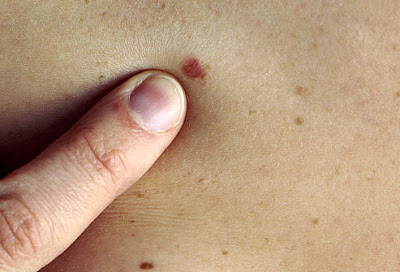
Basal cell carcinoma (BCC) typically manifests as a flesh-colored, pearly bump or a pinkish patch of skin that may resemble a scar. It can also appear as a shiny, translucent bump with visible blood vessels or as a scaly or crusty sore that does not heal. BCC lesions often develop on sun-exposed areas such as the face, ears, neck, scalp, shoulders, and back, but they can occur anywhere on the body. As the tumor grows, it may ulcerate, forming an open sore that may bleed or ooze. BCC lesions generally grow slowly and rarely metastasize to other parts of the body, but they can cause local tissue destruction if left untreated. It’s essential to seek medical evaluation for any suspicious skin changes to ensure early detection and appropriate treatment of basal cell carcinoma.
How is basal cell carcinoma prevented and treated?
Prevention of basal cell carcinoma (BCC) primarily involves minimizing exposure to ultraviolet (UV) radiation. This includes wearing protective clothing, such as wide-brimmed hats and long-sleeved shirts, seeking shade during peak sunlight hours, and regularly applying broad-spectrum sunscreen with a high SPF. Additionally, avoiding tanning beds and sunlamps can help reduce the risk of developing BCC. Regular skin examinations and self-checks are also crucial for early detection and treatment of any suspicious lesions.
Treatment options for basal cell carcinoma vary depending on factors such as the size, location, and aggressiveness of the tumor. Common treatment modalities include:
- Surgical excision: The removal of the tumor and a surrounding margin of healthy tissue is typically the primary treatment for BCC. This can be done through various techniques, including traditional surgery or Mohs micrographic surgery, which involves precise removal and examination of thin layers of tissue until no cancer cells are detected.
- Cryotherapy: Freezing the cancerous cells using liquid nitrogen to destroy them.
- Curettage and electrodesiccation: Scraping away the tumor with a sharp instrument (curette) followed by cauterization with an electric needle.
- Radiation therapy: Using high-energy X-rays to kill cancer cells, particularly for tumors that are difficult to treat surgically.
- Topical medications: Prescription creams or gels containing drugs like imiquimod or fluorouracil may be used to treat superficial BCCs.
- Photodynamic therapy (PDT): A combination of light and a photosensitizing agent to destroy cancer cells.
The choice of treatment depends on factors such as the size and location of the tumor, the patient’s overall health, and their preferences. It’s essential for individuals diagnosed with basal cell carcinoma to work closely with their healthcare providers to develop a personalized treatment plan that best meets their needs and ensures optimal outcomes.